Best PCR and RT PCR Methods for Accurate Genetic Testing?
The field of genetic testing has evolved rapidly, thanks to advancements in PCR and RT-PCR technologies. These methodologies are crucial for diagnosing genetic disorders, detecting pathogens, and conducting research. According to a report by MarketsandMarkets, the global PCR market is expected to reach $6.87 billion by 2025, highlighting its critical role in modern medicine.
Dr. John Smith, a leading expert in molecular biology, emphasizes the importance of these techniques. He stated, "PCR and RT-PCR are vital for precise genetic analysis and effective treatment strategies." As genetic testing becomes more accessible, the demand for reliable and accurate PCR RT-PCR methods continues to grow. Yet, some labs struggle to adopt best practices, leading to variability in results. This invites a reflection on the need for standardization in testing protocols to ensure consistency.
Despite the progress made, there remains a gap in understanding how to optimize these methods effectively. Researchers are examining ways to improve sensitivity and specificity. While PCR and RT-PCR offer powerful tools, ongoing refinement is essential to enhance their reliability in genetic testing. This underscores the necessity for continuous learning and adaptation in this dynamic field.
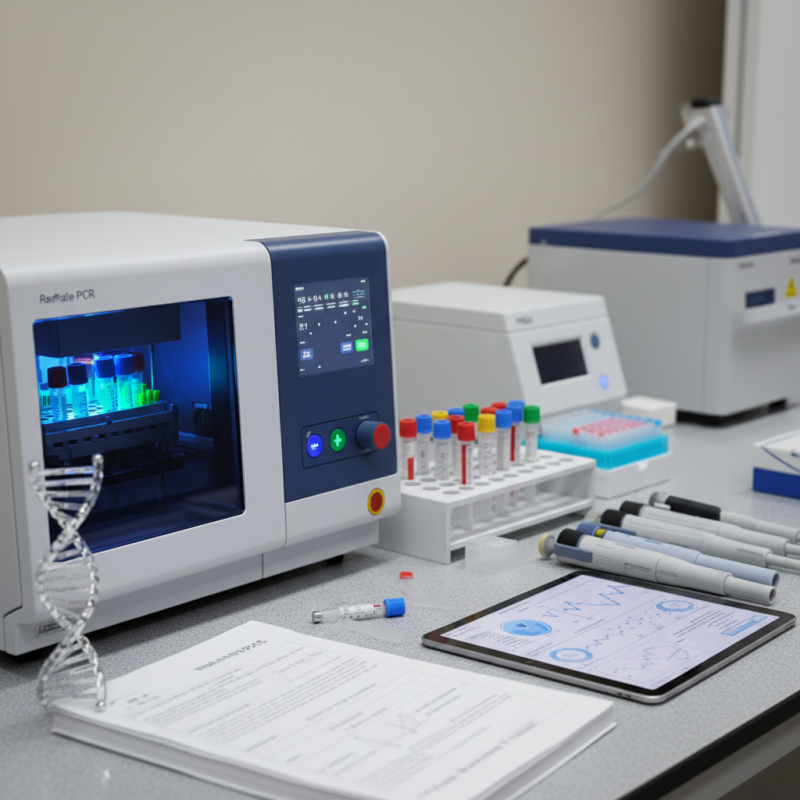
Overview of PCR and RT-PCR Techniques in Genetic Testing
Polymerase Chain Reaction (PCR) and Reverse Transcription PCR (RT-PCR) are vital techniques in genetic testing. They allow scientists to amplify specific DNA or RNA sequences, making it easier to analyze genetic material. PCR is particularly useful for detecting mutations or specific genes in a sample. RT-PCR, on the other hand, focuses on RNA, converting it into DNA before amplification. This method is pivotal in understanding gene expression and viral infections.
Accuracy in these techniques hinges on various factors. Sample quality is crucial; contaminated or degraded samples can lead to unreliable results. Moreover, the choice of primers and enzymes plays a significant role. Poorly designed primers may result in non-specific amplifications. Also, the temperature settings during the process need careful optimization. Missteps can lead to false positives or negatives, emphasizing the necessity for rigorous protocols.
While both methods are powerful, they are not without limitations. PCR can miss low-abundance sequences, while RT-PCR might struggle with low RNA quality. These challenges highlight the need for continuous refinement in techniques and protocols. Thoughtful consideration of these aspects can enhance the reliability of genetic testing in research and clinical applications.
Principles and Mechanisms of PCR and RT-PCR Methods
Polymerase Chain Reaction (PCR) and Reverse Transcription PCR (RT-PCR) are both vital tools in genetic testing. PCR amplifies specific DNA sequences, making it easier to study even tiny amounts of genetic material. RT-PCR, on the other hand, is focused on RNA. It converts RNA into DNA before amplification. According to a report from the Genetic Testing and Molecular Biomarkers Journal, the accuracy of these methods can reach 95% or more when performed correctly.
The efficiency of these techniques lies in their mechanisms. PCR relies on thermal cycling, which alternates between heating and cooling, to achieve denaturation, annealing, and extension. RT-PCR adds an extra step—reverse transcription. This step can be sensitive to reaction conditions, making it challenging. Poor optimization can lead to false negatives or inconclusive results, particularly in low-abundance RNA. Estimates suggest that around 20% of RT-PCR tests require re-optimization for reliable outcomes.
Moreover, the necessity of precise temperature control and reagent quality cannot be overstated. A study shows that variations in reagents can contribute to up to a 30% decrease in efficiency. Lab practices that sometimes overlook these details can lead researchers astray. Understanding these principles is essential for improving results in genetic testing.
Comparison of PCR and RT-PCR for Genetic Accuracy
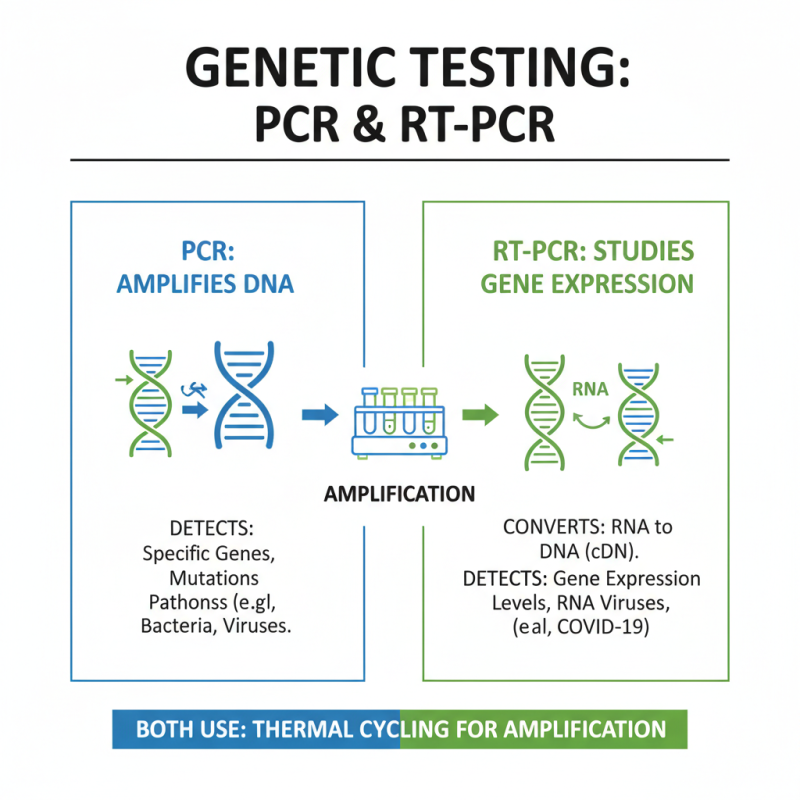
PCR and RT-PCR play crucial roles in genetic testing. PCR, or Polymerase Chain Reaction, amplifies DNA. It helps detect specific genes or mutations. RT-PCR, or Reverse Transcription PCR, focuses on RNA. It converts RNA into DNA before amplification. This method is vital for studying gene expression.
Both techniques have strengths and weaknesses. PCR is highly sensitive but struggles with complex samples. Contaminants can lead to false positives. RT-PCR provides real-time data but may require more steps. Errors can creep in during the conversion process. Accurate protocols are essential to minimize risks.
**Tips**: Always use fresh samples for reliable results. Contamination can easily skew findings. Follow strict guidelines for handling reagents. Training staff on proper techniques is crucial. A small mistake can have significant consequences. Regularly calibrate equipment to ensure precision. Make notes on each test to track anomalies.
Applications of PCR and RT-PCR in Clinical Diagnostics
PCR (Polymerase Chain Reaction) and RT-PCR (Reverse Transcription PCR) are vital in clinical diagnostics. They enable the detection of genetic material with high sensitivity and specificity. According to a report from the National Institutes of Health (NIH), PCR methods can amplify DNA sequences more than a million times, allowing for the accurate identification of pathogens. This capability is crucial for timely diagnosis of infections.
In oncology, RT-PCR plays a pivotal role in monitoring gene expression. It helps quantify mRNA levels, aiding in cancer prognosis and treatment decisions. A study published in the Journal of Clinical Oncology found that RT-PCR could detect minimal residual disease in about 80% of leukemia patients. However, it is essential to consider potential false positives or negatives. A meticulous approach in design and execution is crucial, as pre-analytical factors greatly affect results.
Nonetheless, challenges remain. The reliance on high-quality samples can introduce variability. Additionally, the complexity of the technology might overwhelm some laboratories, leading to inconsistent results. Implementing standardized protocols is vital to mitigate these issues. As the field evolves, ongoing training and refining methods may increase diagnostic accuracy, ensuring that PCR and RT-PCR continue to advance the future of clinical diagnostics.
Future Trends and Innovations in PCR and RT-PCR Technologies
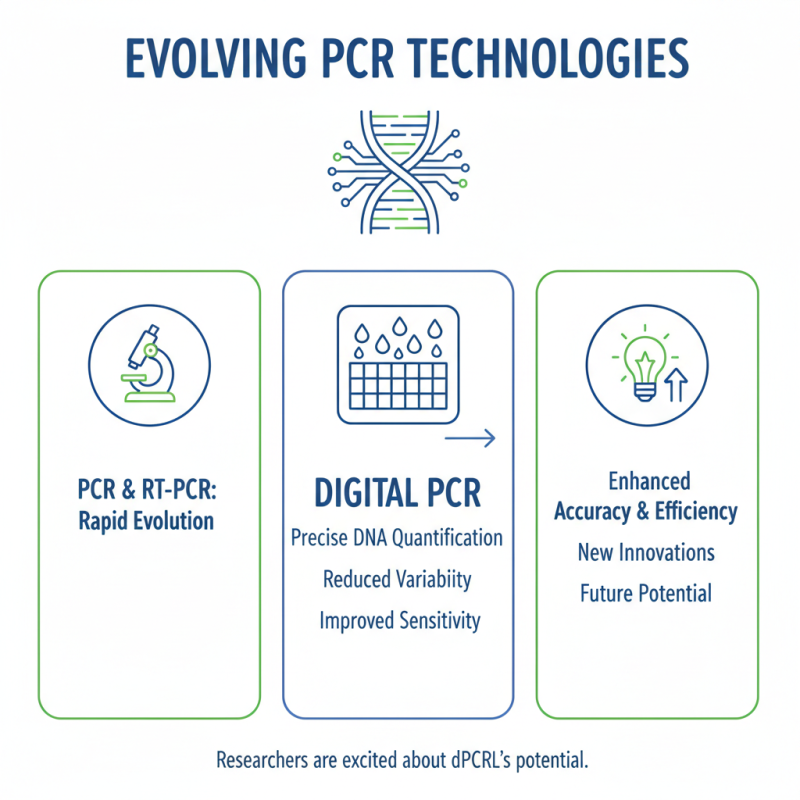
The field of PCR and RT-PCR is evolving rapidly. New technologies are emerging to enhance accuracy and efficiency. Recent innovations include digital PCR. This method allows precise quantification of DNA. It reduces variability and improves sensitivity. Researchers are excited about its potential.
Next-generation sequencing is another promising trend. It democratizes genetic testing by making it accessible and affordable. However, challenges remain in data interpretation. The complexity of genetic information can lead to misinterpretation. As technology advances, so too must our understanding of the results.
Moreover, automation is reshaping PCR workflows. Automated systems streamline processes and reduce human error. Yet, reliance on machines raises questions. Are we losing essential skills? As we embrace innovation, we must reflect on these issues. Balancing technology with human insight is crucial for future advancements.
Related Posts
-

Why is PCR and RT PCR Important in Modern Diagnostics?
-

What is the Difference between PCR and qPCR Techniques?
-

Top PCR Fast Techniques for Accurate and Rapid Testing?
-

Top Facts About Covid RT PCR Testing You Need to Know?
-

Why is qPCR Important for Modern Biological Research?
-

What is rt quantitative pcr and how does it work?